4 Wake-Up Calls Every Woman Needs to Improve Her Health
Women’s health is finally getting the attention it deserves. We’re talking about once-taboo topics like menopause, mental health, caregiver burnout, and chronic pain—with each other and with our doctors. Yet many of us still feel overwhelmed and unsure where to focus our attention when it comes to protecting our health, according to a groundbreaking new national report from the Cleveland Clinic Women’s Health and Research Center.
Some of the findings are hard to ignore and should alarm us all, says Maria Shriver, the center’s chief visionary and strategic advisor. “But there is also hope in these findings. We know that information and research is power, and we need to keep fighting for both.”
The best place to start: Understanding this new report’s most eye-opening findings, which point to clear opportunities for all of us to take charge of our health now. Here are four of the most important takeaways, and the small but meaningful actions experts say can make a real difference.
In this article, you’ll learn...
- Exactly what to ask if financial worries are preventing you from getting the care you need
- Why gynecologic care is essential no matter how old you are (or whether you’re sexually active)
- The surprising ways menopause impacts your future health
- Evidence-based action steps you can take to improve your brain health now and for years to come
Takeaway No. 1: Too many women are more worried about affording healthcare than developing serious health issues.
As anyone who has faced steep medical bills and increasing insurance and healthcare costs knows all too well, the stress that comes along with paying for healthcare is real. Not surprisingly, that worry about finances is preventing many of us from getting the care we need and deserve.
Nearly half of women polled said their biggest concern as they age is not having enough money to take care of their health. In fact, it’s a bigger worry than the threat of developing cancer, heart disease, or Alzheimer’s. However, financial concerns keep women from being proactive about their health: Women who consider their financial health “fair/poor” are more likely to admit that they aren’t taking any preventive measures to support their cognitive health than those who consider their financial health “excellent/very good.”
What you can do: Know that under the Affordable Care Act, many preventive services (such as annual wellness visits, mammograms, cervical cancer screening, birth control, and more) should be covered without copays or insurance deductibles. You can call a provider’s office and ask which preventive services are fully covered under your plan, or ask if a telehealth visit might reduce your cost. You can also ask for a “cash-pay” price, which can be less expensive than going through insurance, or look into hospital financial assistance programs.
While it can feel tough to talk about money concerns at a healthcare visit, your clinician will want you to bring it up—and can likely help you navigate the system. After all, avoiding or postponing care because of cost can create bigger health (and financial) crises later on.
“Women spend about $15.4 billion more than men annually on out-of-pocket healthcare costs.”
Takeaway No. 2: Annual, preventive care is too often overlooked—especially as women age.
Think you can skip seeing a primary care provider every year if you’re healthy? You’re not alone: Nearly one-third of women polled don’t feel the need to go because they’re generally healthy. For 26 percent of women, anxiety is what prevents them from making that annual PCP appointment.
Similar gaps in understanding exist when it comes to an annual well woman exam with a gynecologist, with a majority of women reporting not having seen an ob/gyn or other gynecologist specialist in the past year:
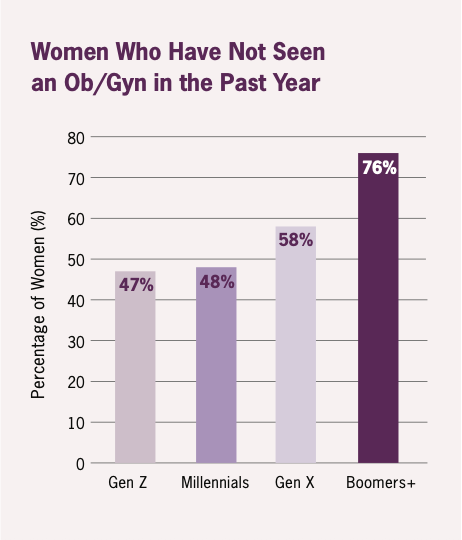
Why? Four in 10 women overall (and nearly 60 percent of Boomers+) say they don’t believe an annual gynecologic visit is necessary, with 22 percent of women operating under the misconception that gynecologists are only needed for pregnancy planning and care.
What you can do: It’s crucial to understand that an annual gynecologic visit covers much more than pregnancy and is important for women of all ages. One important reason: These are the preventive appointments where you’ll be screened for gynecologic cancers, and your risk for these cancers increases with age, says Beri Ridgeway, MD, executive vice president and chief of staff of Cleveland Clinic and co-founder of the Cleveland Clinic Women’s Comprehensive Health and Research Center. “Routine care makes a difference in early cancer detection,” she says.
Finding a gynecologist you feel comfortable talking to about the more intimate aspects of your health is also key. Ask friends or colleagues who they see and like, and “interview” a new clinician during that first appointment to make sure they feel like the right clinician for you.
Takeaway No. 3: The menopause transition impacts your heart, brain, and bones in profound ways.
Whether you sailed through menopause with few symptoms or suffered through hot flashes, sleepless nights, or other symptoms, most women feel grateful when the menopause transition is behind them—and they think it can stay in the rearview. Yet this major hormonal transition influences multiple aspects of a woman’s future health outcomes, and too many of us don’t realize this. In fact, more than two in five women reported being unaware that menopause can affect the heart, brain, and bones.
What’s more, a majority of the women polled said menopause isn’t discussed enough, and more than a third weren’t aware of the various menopause treatment options available, including hormone therapy, adjustments to lifestyle, supplements, and more.
In short: Despite more talk about menopause these days, it’s one of the most misunderstood transitions in a woman’s life.
“We see many women who have not felt heard or pushed down the wrong path when managing their menopause transition,” says Pelin Batur, MD, medical director of the Cleveland Clinic Women’s Comprehensive Health and Research Center. “To navigate this transition, women need accurate information from trained medical professionals in an environment where they feel comfortable talking about what they’re experiencing.”
What you can do: Ideally, find a menopause specialist who understands this major hormonal transition in nuanced ways. The Menopause Society has a searchable directory that can help you find a specialist. That said, many clinicians who don’t have a specific menopause certification can still help you navigate your health in midlife and beyond.
Some of the “green flags” to look for in a menopause clinician are someone who takes a detailed symptom history; talks about sleep, mood, heart health, brain health, and bone health; discusses risks and benefits of treatment options; and prioritizes shared decision-making.
Takeaway No. 4: Two-thirds of people diagnosed with Alzheimer’s disease are women—yet most of us don’t know this.
When asked whether men or women are more likely to get Alzheimer’s disease, just 19 percent of women polled answered correctly—and only 29 percent said they worry they may get the disease when they’re older. This lack of awareness that women disproportionately suffer from Alzheimer’s and lack of concern that we’ll develop the disease mean too many of us don’t even have dementia on our radar. That’s a shame, considering there are proven steps we can take to reduce our risk of this devastating disease. (More on those below.)
The truth is that with more knowledge comes a sense of empowerment—and action. In that same poll, nearly nine in 10 of those who know women are at higher risk than men for Alzheimer’s are taking preventive measures to support their brain health.
What you can do: So, what are some of those proven ways to protect our cognitive health as we age? Research commissioned by The Lancet identified 14 potentially modifiable factors that account for 45 percent of cases of dementia, including less education; hearing loss; high LDL cholesterol (the “bad” kind); depression, traumatic brain injury; physical inactivity; diabetes; smoking; hypertension; obesity; excessive alcohol consumption; social isolation; air pollution; and vision loss.
That study also found that addressing these between ages 18 and 65 had the greatest impact in delaying and even preventing the onset of dementia.
Translation: Things like treating high cholesterol and depression, exercising regularly, quitting smoking, and prioritizing community really can make a difference when it comes to your brain health.
Download the 2026 State of Women's Health Report here!


Answer
The letter "M"
Please note that we may receive affiliate commissions from the sales of linked products.




